New evidence provides a stronger link between chronic anxiety and future neurocognitive decline, demanding a re-evaluation of how we approach dementia prevention in clinical practice.
A major updated meta-analysis, now available in the Journal of Clinical Medicine, confirms that anxiety is significantly associated with an increased risk of all-cause dementia. This extensive study, spanning nine prospective cohorts and representing 29,608 participants, offers crucial clarity on this controversial topic.
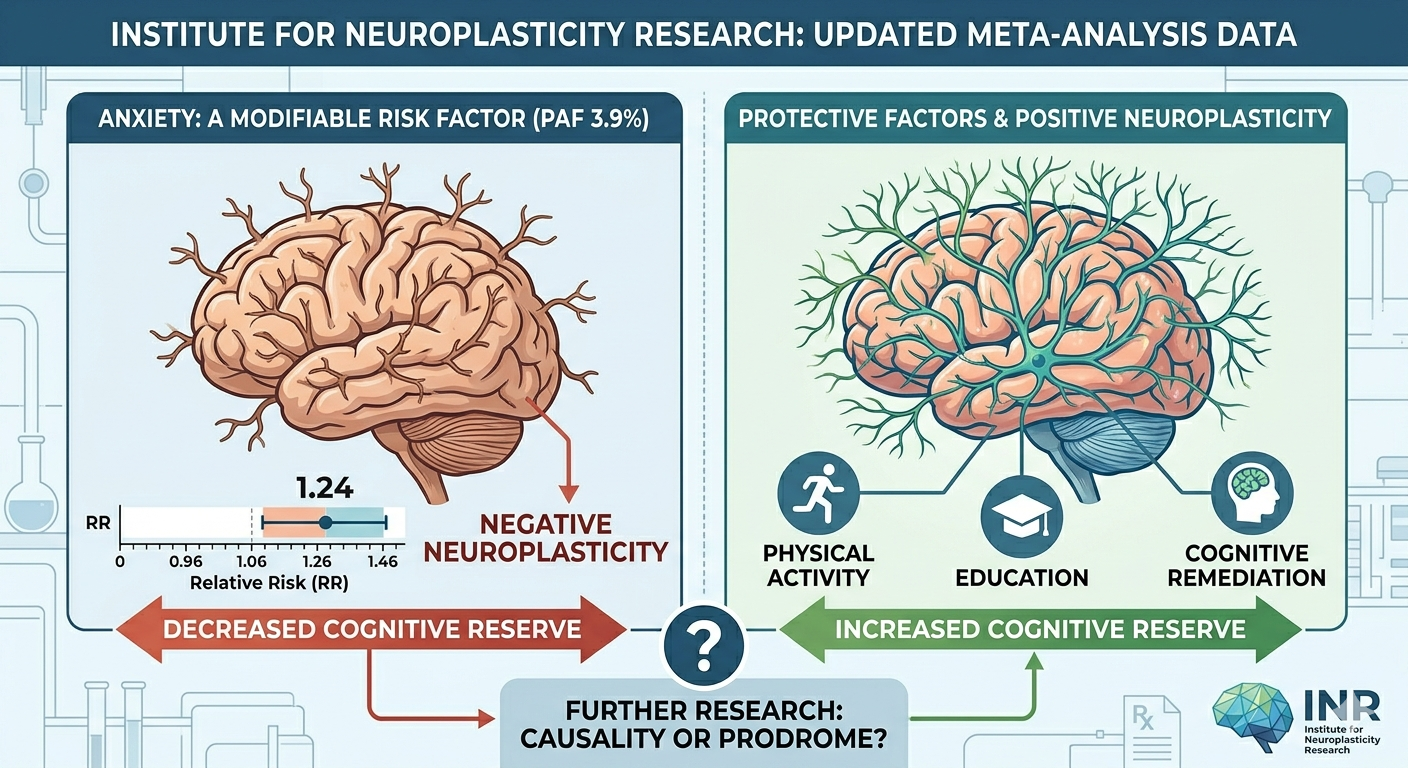
The data revealed a pooled Relative Risk (RR) of 1.24 (95% CI: 1.06-1.46). Even more compelling is the estimated Population Attributable Fraction (PAF), which suggests that 3.9% of dementia cases might be prevented if anxiety were effectively managed. This identifies anxiety as a key, potentially modifiable risk factor.
While the causal direction requires further exploration (is anxiety a primary cause or an early prodromal symptom?), the neurobiological implications are clear. Anxiety contributes to mechanisms of “negative neuroplasticity.” This manifests as dendritic atrophy and detrimental morphological changes that actively decrease cognitive reserve.
Our goal must be to identify intervention windows where addressing mental health can directly protect neurological function. Further research into how positive neuroplasticity—strengthened through physical activity, education, and cognitive remediation—can counteract this risk is paramount.
You can access the full paper and full data set here: https://pubmed.ncbi.nlm.nih.gov/32526871/
#Neuroplasticity #Neuroscience #DementiaResearch #Anxiety #CognitiveHealth #ClinicalMedicine #InstituteForNeuroplasticityResearch #RiskFactors



 Posted in
Posted in